OVERVIEW YouTube Video Link: https://youtu.be/yxrdEDPX6QU
Beginning in 1990, the first iteration of this section was provided to all attending and incoming (i.e., Residents & Fellows) Department of Medicine physicians at UWHC. It was also posted at each specialty section office of the Department of Medicine, the Pulmonary outpatient clinic, and updated as new evidence-based information was published. Unlike EHR capabilities today, where this information could easily be a pop-up page, hard copies were initially distributed.….over the years, many trees were sacrificed to disseminate the information.
- This initiative allowed for one of the initial Quality Assurance (QA) projects of the Pulmonary Diagnostic Services; to improve the quality/consistency of delivered services, as well as address the finalization of the capitated reimbursement model that was proposed in 1983.
My intent was to begin the process of providing a clear understanding of the type of testing and indications for the common tests offered by the Pulmonary Diagnostic Services. My hope was that first, this was read by the recipient. Second, that it would reduce confusion and provide consistency in test ordering (reduce variability and improve quality). And third, if the requesting physician received a call by a Pulmonary Diagnostic Technologist questioning the rationale behind a specific order for Pulmonary Diagnostic Testing, they would both be working off the same page regarding what each test had to offer.
Note: The indications listed below may not be entirely consistent with what is recommended today. Therefore, they are for information only. However, the process intent remains the same since inception; providing well-defined description(s) of pulmonary diagnostic test indications.
As can be seen, these are commonly performed Pulmonary Diagnostic tests. The additional services provided (e.g., CPET, Indirect Calorimetry, Shunt Studies, Breath Tests, HAST, Intrapulmonic Gas Distribution, Ventilatory Drives, Resting Frigid Air Bronchoprovocation [with/without Eucapnic Hyperpnea], Pulmonary Compliance, Transdiaphragmatic Pressure Monitoring, Infant Testing, etc.) are not included here since they were primarily of interest to specific sub-specialties, or other HCPs. Listing these additional procedures would have only potentially added to the confusion surrounding what commonly performed Pulmonary Diagnostics offer to overall patient management.
Indications for Pulmonary Diagnostic Testing
A. Spirometry1
The need for
1. detecting the presence or absence of lung dysfunction suggested by history or physical indicatons (e.g., age, smoking history, family history of lung disease, cough) and/or the presence of other abnormal diagnostic tests (e.g., chest x-ray, arterial blood gases)
2. quantify the severity of know lung disease
3. assessing the change in lung function over time, or following administration of, or change of, therapy
4. assessing the potential effects , or response to, environmental exposure
5. assessing the risk for surgical procedures known to affect lung function
6. assessment of impairment and disability (pre-employment evaluations)
B. Spirometry with Bronchodilator (acute response assessment)
The need to assess
1. reversible airflow limitation: based upon spirometric evidence of
a. decreased FEV1 / FVC ratio (< predicted)
b. %predicted FEF25-75 / %predicted FVC < 0.8
c. decreased FEF50% and/or decreased FEF75% with normal PEF and/or FEF25%
2. evidence of central and/or peripheral airways disease
a. increased Raw (> 2.0 cm H2O/L/sec in adults)
b. decreased sGaw (< 0.17 L/sec/cm H2O/L)
3. reversible air-trapping evidenced by
a. increased RV/TLC ratio
C. Maximum Voluntary Ventilation (MVV)
To be employed
1. as a compliance indicator (e.g., post-operatively)
2. to assess respiratory muscle endurance (MVV < FEV1 X 35 with apparent maximal subject effort)
3. as a predictor of exercise VEMAX
4. to assess airway hyperreactivity
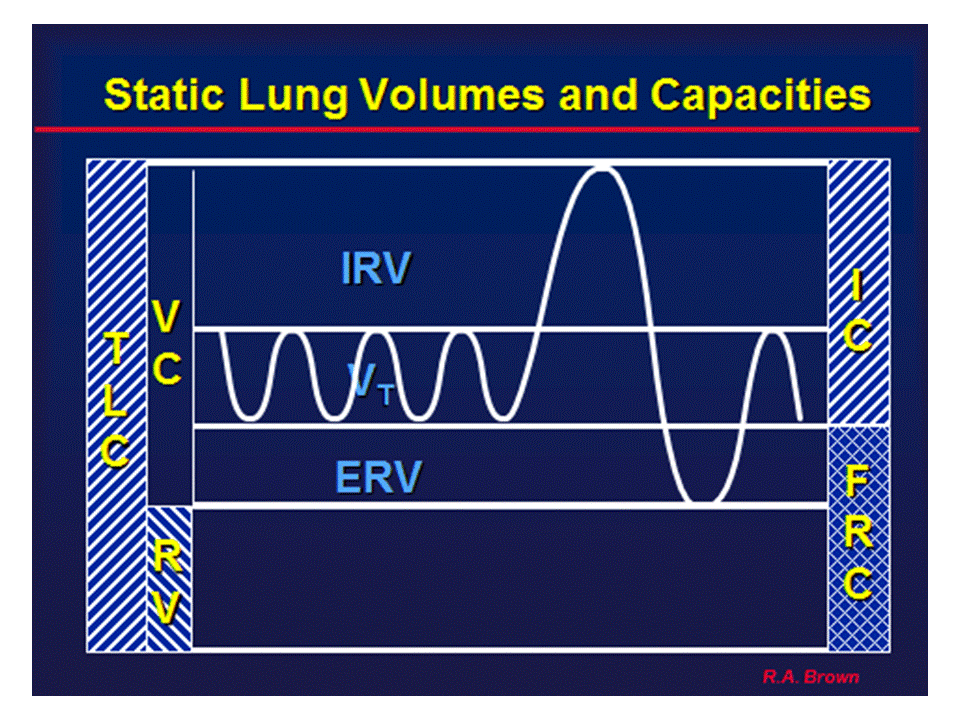
D. Static Lung Volumes
The need to
1. differentiate between obstructive and restrictive disease patterns2
a. VC and/or FVC < 80% predicted and/or < LLN; FVC with/without evidence of airflow limitation
2. rule out and/or quantify trapped gas5
a. increased RV/TLC ratio
3. assess response to therapeutic intervention (e.g., respiratory medications, radiation, transplantation, chemotherapy, lobectomy)2
4. quantify the presence and amount of unventilated lung (Open- or Closed-Circuit vs Plethysmographic methods)
5. assess effects of chronic disease (e.g., sarcoidosis, rheumatoid and uremic lung)
6. make preoperative assesments2 for upper abdominal or thoracic procedures
7. evaluate pulmonary disability
8. aid in the interpretation of other lung function tests2
E. Airway Mechanics (Raw, Gaw, sGaw)
The need to
1. differentiate types of obstructive patterns having similar spirometric configuration
2. differentiate sites of airway obstruction
a. central vs peripheral airway components
3. assess response to therapeutic intervention
a. bronchodilator (acute or chronic)
b. anti-inflammtory medications (e.g., steroids)
4. assess the magnitude of response to a bronchoprovocative agent
F. Diffusing Capacity3
1. Evaluation and follow-up of parenchymal diseases associated with dusts (e.g., asbestos) or drug reactions (e.g., amiodarone) or related to sarcoidosis;
2. Evaluation and follow-up of emphysema and cystic fibrosis;
3. Differentiating among chronic bronchitis, emphysema and asthma in subjects presenting with airflow limitation;
4. Evaluation of pulmonary involvement in systemic diseases (e.g., rheumatoid arthritis, systemic lupus erythematosus);
5. Evaluation of cardiovascular disease (e.g., primary pulmonaryhypertension, pulmonary edema, acute or chronic thromboembolism);
6. Prediction of arterial desaturation during exercise on subjects with COLD;
7. Evaluation and quantification of disability associated with interstitial lung disease;
8. Evaluation of the effects of chemothreapy agents, or other drugs known to induce pulmonary dysfunction;
9. Evaluation of hemorrhagic disorders.
G. Arterial Blood Gas Analysis and Hemoximetry4
The need to
1. evaluate the adequacy of a subject’s ventilatory (PaCO2). acid-base (pH and PaCO2), and/or oxygenation (PaO2 and O2Hb) status, and the oxygen-carrying capacity (PaO2, O2Hb, tHb and dyshemoglobin saturations) and intrapulmonary shunt (QSP/QT).
2. quantitate the response to therapeutic intervention (e.g., supplemental oxygen administration, invasive and/or non-invasive ventilatory support) and/or diagnostic evaluation (e.g., exercise desaturation).
3, to monitor severity and progression of documented disease processes.
H. Maximal Occluding Pressures (lung volume adjusted)
The need to assess
1. the presence and magnitude of respiratory muscle weakness
a. acute and chronic
2. the effect(s) of lung hyperinflation
3. response to therapeutic intervention
a. nocturnal ventilation
b. inspiratory muscle training
c. medications
d. nutrition
I. Bronchial Provocation6
The need to
1. diagnose or to confirm a diagnosis of airway hyperreactivity
2. follow changes in airway hyperresponsiveness
3. document the severity of airway hyperresponsiveness
4. determine who is at risk in the military or workplace
5. establish a control or baseline prior to a series of environmental or occupational exposures
References
1. American Association for Respiratory Care Clinical Practice Guideline: Spirometry. Resp Care 1991;36:1414-1417.
2. American Association for Respiratory Care Clinical Practice Guideline:Static Lung Volumes. Respir Care 1994;39:830-836.
3. American Association for Respiratory Care Clinical Practice Guideline: Single-Breath Carbon Monoxide Diffusing Capacity. Respir Care 1993;38:511-515.
4. American Association for Respiratory Care Clinical Practice Guideline: In-Vitro pH and Blood Gas Analysis and Hemoximetry. Respir Care 1993;38:505-510.
5. American Association for Respiratory Care Clinical Practice Guideline: Total Body Plethysmography. Respir Care 1994;39:1184-1190.
6. American Association for Respiratory Care Clinical Practice Guideline: Bronchial Provocation. Respir Care 1992;37:902-906.
Go to Review of Services at: https://pftlabresources.com/review-of-services-offered-by-pulmonary-diagnostic-laboratory/